From: Rosalie Wyonch
To: Canadians concerned about long-term care
Date: August 30, 2021
Subject: Learning from Deadly Lessons: Seniors' Care and COVID-19
The impact of COVID-19 on Canadian seniors, in particular for residents of long-term care and retirement homes, has been devastating.
With more than 15,000 resident and 30 staff deaths, Canadians are expecting governments to improve residential seniors’ care after the pandemic. This will require strategic modernization of seniors’ care and the long-term care sector in particular to address myriad complex and interrelated policy issues.
Though it might be easiest to name and shame the facilities with high mortality and lay blame on their managers, such scapegoating does nothing to address real and broader problems in the residential care sector, which includes independent-living, retirement and long-term care facilities.
Despite significant efforts from frontline staff, residential care administration and government, almost half (47 percent) of Canada’s LTC and retirement homes experienced an outbreak. Recent analysis by Statistics Canada shows that critical staff shortages, the size of residential care facilities and having an employee test positive for COVID-19 were associated with a higher likelihood of having at least one resident infected.
Contrary to many commentators and media reports, for-profit residential care homes in Canada were not significantly more likely to have a COVID-19 outbreak than non-profit homes. Similarly, other research analyzing Ontario, in particular, from the first wave of the pandemic also showed that for-profit homes were no more likely than non-profit homes to experience an outbreak. Though the extent of outbreaks and associated mortality was higher in for-profit homes, the difference was explained by older design standards (pre-1972, facilities allowing four beds per room) and chain ownership. Facilities with chain ownership are also more likely to be larger facilities with older design standards, meaning that causality of worse outbreaks is still relatively unclear, although single rooms had fewer cases in adult living settings. Insights from these and other research reports suggest that the size and layout of facilities in addition to staffing pressures are critical challenges that must be addressed.
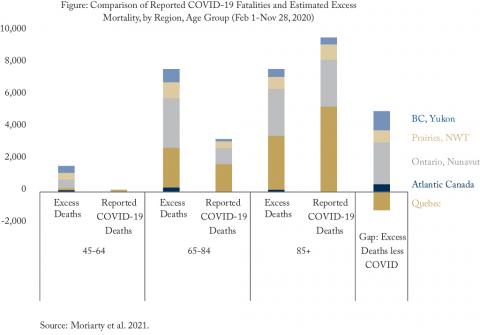
New data and information can also fundamentally alter our understanding of the pandemic’s effects on seniors: research on excess mortality data suggests that at least two-thirds of deaths (~6,000) caused by COVID-19 in communities (outside of long-term care) may have been missed in official counts. In particular, many clinically frail older adults succumbed to COVID-19 in their own homes, racialized and low-income communities were disproportionately affected by COVID-19, and more deaths occurred in the working age populations (45-64 years) than official case and mortality statistics suggest (see Figure).
There is significant uncertainty about the true effects of COVID on Canada’s senior population. Case and mortality data is likely most complete in the institutional residential settings of LTC and retirement homes. The uncertainty and missing information provide a biased impression that seniors living in the community were much less affected than they really were: only four in 10 excess deaths in the population 65 to 84 were attributed to COVID.
Upgrading existing infrastructure, recruiting and training healthcare providers and improving access to care in the community, particularly for seniors and those in low-income and racialized communities are all challenges that existed before the pandemic. Long waitlists for residential care were an issue prior to the pandemic and as Canada’s population continues aging, we need every bed we have and more.
Unless policymakers, health sector stakeholders, managers, politicians and care providers can mount a coordinated sustained effort to address these well-known challenges, they will persist after the pandemic as well.
Rosalie Wyonch is a Senior Policy Analyst at the C.D. Howe Institute.
To send a comment or leave feedback, email us at blog@cdhowe.org.
The views expressed here are those of the author. The C.D. Howe Institute does not take corporate positions on policy matters